Staying engaged in class can sometimes feel like an uphill battle.
With distractions lurking around every corner and the ebb and flow of thoughts competing for attention, it’s no surprise that many students find their minds wandering.
However, there are gentle, effective ways to cultivate a more engaged mindset during those learning sessions.
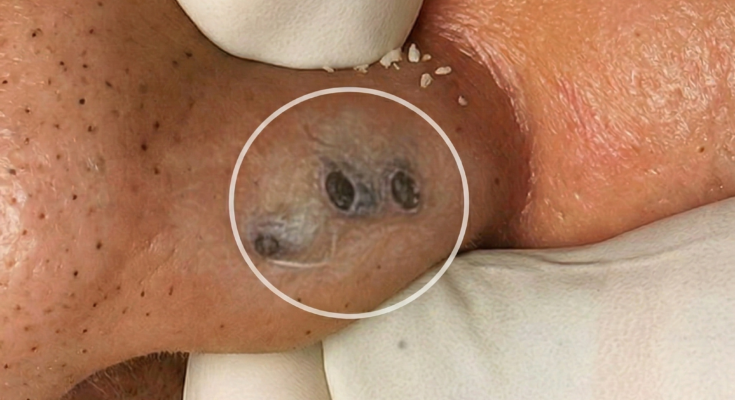
Managing mild to moderate comedonal acne at home begins with understanding how these lesions form. Comedonal acne develops when excess sebum combines with dead skin cells inside the hair follicle, leading to clogged pores. This process, known as abnormal follicular keratinization, causes cells that would normally shed to accumulate and form a plug. When the pore remains closed, it appears as a whitehead. When the plug is exposed to air and oxidizes, it becomes a blackhead. Unlike inflammatory acne, comedones are primarily driven by congestion rather than infection, although untreated blockages can eventually trigger inflammation.
Several internal and external factors can contribute to this buildup. Increased sebum production, often influenced by hormonal fluctuations, can make pores more prone to clogging, particularly in individuals with oily skin. Genetic predisposition also plays a role in pore size, oil production, and skin cell turnover. Skincare habits may further influence comedonal acne. Overly harsh cleansing, aggressive physical exfoliation, or frequent use of multiple active ingredients can disrupt the skin barrier, which may worsen congestion over time. Environmental factors such as humidity, occlusive cosmetics, and heavy hair products around the hairline can also contribute to persistent blackheads and whiteheads.
Effective home management focuses on normalizing cell turnover while supporting the skin barrier. Topical retinoids are commonly recommended because they help regulate keratinization and reduce the formation of new comedones. Over-the-counter retinoids such as adapalene may improve clogged pores gradually when used consistently. Salicylic acid, a beta hydroxy acid, is oil-soluble and can penetrate into pores to dissolve accumulated debris, making it particularly helpful for blackheads. Niacinamide may support oil regulation and barrier function, while lightweight, non-comedogenic moisturizers help prevent dehydration that can otherwise trigger compensatory oil production. Gentle cleansing twice daily is typically sufficient, as excessive washing can impair barrier integrity and increase irritation.
Benzoyl peroxide is often associated with inflammatory acne but may also be used in mild to moderate cases where comedones coexist with occasional papules or pustules. However, because comedonal acne is primarily driven by clogged pores rather than bacterial overgrowth, keratolytic and retinoid-based approaches are usually central. Introducing one active ingredient at a time and allowing several weeks for adjustment can reduce the likelihood of irritation, which itself can worsen congestion if the skin barrier becomes compromised.
For individuals who do not see improvement after consistent use of over-the-counter treatments for several months, professional evaluation may be appropriate. Dermatologists may prescribe stronger topical retinoids or recommend procedures such as professional comedone extraction or chemical peels when suitable. Persistent or worsening acne should always be assessed by a qualified medical professional to rule out underlying hormonal influences or other dermatologic conditions.
Realistic expectations are essential. Comedonal acne often improves gradually, as treatments work by preventing new blockages rather than instantly clearing existing ones. Visible changes may take eight to twelve weeks of consistent use. Overuse of active ingredients can lead to irritation, dryness, and barrier disruption, which may delay progress. A steady, evidence-informed routine that balances exfoliation with barrier support is generally more effective than frequent product changes. Educational guidance grounded in acne biology, as emphasized in professional dermatology-based skincare frameworks, supports long-term skin health while minimizing unnecessary risk.