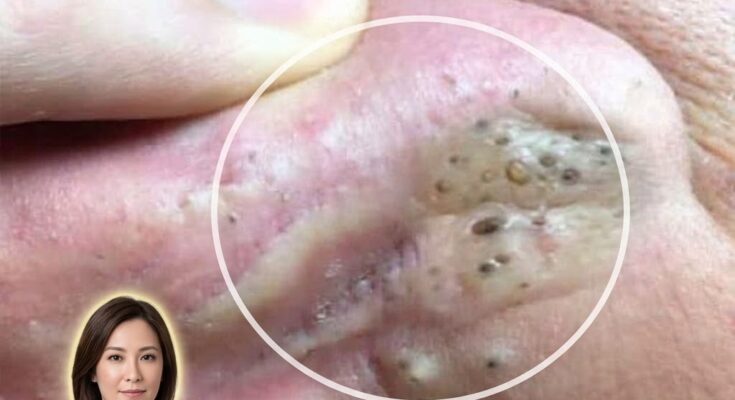
Follicular keratinization is a central biological process involved in the development of acne. Inside each hair follicle, skin cells known as keratinocytes are continuously produced and shed as part of normal skin renewal. In healthy skin, these cells gradually move upward and are released from the pore opening. In acne-prone skin, however, this shedding process can become disrupted. Keratinocytes may accumulate and stick together instead of separating normally. When these excess cells mix with sebum, the oily substance produced by sebaceous glands, they can form a plug within the follicle. This microscopic blockage is often the first stage of acne formation and may develop into comedones such as blackheads and whiteheads.
As the follicle becomes obstructed, sebum continues to be produced by the oil gland attached to the pore. Because the plug limits normal flow to the skin surface, oil begins to collect within the follicle. This environment may encourage the growth of Cutibacterium acnes, a bacterium that naturally lives on the skin. The combination of trapped oil, accumulated keratinocytes, and bacterial activity can create internal pressure inside the pore. Over time, this may lead to visible comedones or progress toward inflammatory acne lesions if the follicle wall becomes irritated or ruptures.
Several factors can influence abnormal follicular keratinization. Hormonal activity plays an important role, particularly during adolescence or hormonal fluctuations in adulthood. Increased androgen activity can stimulate larger sebaceous glands and higher sebum production, which may worsen pore congestion when keratinocytes are not shedding efficiently. Genetic predisposition may also affect how quickly skin cells turn over or how easily they adhere to one another within the follicle. In addition, certain cosmetic products, heavy occlusive ingredients, or incomplete cleansing may contribute to the buildup of debris on the skin surface that can worsen clogged pores.
Skincare habits and environmental influences may further affect this process. Excess oil production associated with oily skin can increase the likelihood that accumulated skin cells will combine with sebum to form a follicular plug. Humidity, sweat, and exposure to certain hair or skincare products may also contribute to congestion in susceptible individuals. Mechanical factors such as frequent touching of the skin or squeezing existing lesions may disrupt the follicle structure and worsen inflammation around already blocked pores.
Because follicular keratinization is a primary driver of comedone formation, many acne treatments are designed to normalize the way skin cells shed inside the follicle. Topical retinoids are commonly recommended in dermatology because they help regulate keratinocyte turnover and reduce the tendency for cells to accumulate within pores. By promoting more consistent cell renewal, retinoids may help prevent the formation of new blackheads and whiteheads over time. Salicylic acid is another widely used ingredient that can penetrate into oil-filled pores and help loosen the mixture of sebum and dead skin cells contributing to congestion.
Additional ingredients may support acne-prone skin by targeting other parts of the acne process. Benzoyl peroxide is often used to reduce acne-causing bacteria and inflammation within clogged follicles. Niacinamide may help support the skin barrier and reduce excess oil production in some individuals. Gentle cleansing routines and non-comedogenic skincare products are commonly recommended to minimize additional pore blockage while maintaining the skin’s natural barrier function.
Professional dermatology treatments may also be considered when acne persists despite over-the-counter care. Prescription retinoids, combination topical therapies, chemical peels containing salicylic acid or other exfoliating agents, and in some cases oral medications may be used to manage more severe acne linked to abnormal follicular keratinization. These treatments are typically selected based on the severity of acne, skin type, and individual response to therapy.
Although treatments may help improve the shedding of skin cells within follicles, the underlying tendency toward follicular keratinization can remain a long-term characteristic of acne-prone skin. For this reason, ongoing maintenance skincare is often recommended to help keep pores clear and reduce the likelihood of new breakouts. Individuals experiencing persistent, painful, or scarring acne are generally encouraged to seek guidance from a qualified dermatologist, who can provide a treatment plan tailored to the biology of their skin.