Studying can often feel like a daunting task, especially in our fast-paced world filled with distractions.
Many of us find ourselves wrestling with our thoughts, unable to concentrate on the material at hand.
However, with a few gentle adjustments to our habits and environment, we can cultivate a more focused mindset that makes studying not only easier but also more enjoyable.
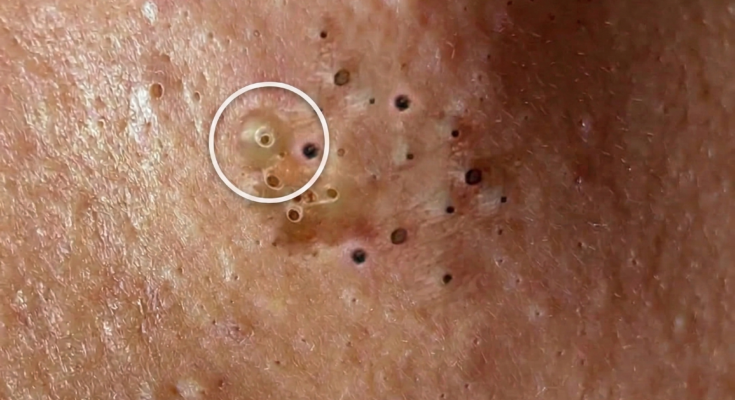
Understanding the microenvironment inside acne-prone pores requires examining the biological processes occurring within the hair follicle. Each pore is connected to a sebaceous gland that produces sebum, an oily substance designed to lubricate and protect the skin. In individuals prone to acne, this environment can shift in ways that encourage pore blockage and inflammation. Excess sebum production, combined with abnormal shedding of skin cells through a process known as follicular keratinization, creates conditions where dead cells and oil accumulate inside the follicle. As this material builds up, it can form a microcomedone, which is considered the earliest stage of both blackheads and whiteheads.
Within this confined space, several biological factors interact to shape the pore’s microenvironment. Sebum provides a lipid-rich medium that can support the growth of certain skin bacteria, including Cutibacterium acnes. While this bacterium is a normal resident of the skin, an overgrowth within clogged pores may contribute to inflammatory signaling. At the same time, limited oxygen inside blocked follicles creates an environment that favors bacterial proliferation. The combination of trapped sebum, compacted keratinocytes, and bacterial activity can stimulate immune responses that lead to redness, swelling, and the formation of inflammatory acne lesions.
Hormonal activity is another major influence on the internal environment of acne-prone pores. Androgens stimulate sebaceous glands to produce more sebum, which can increase the likelihood of pore congestion. Hormonal fluctuations during adolescence, menstrual cycles, or periods of stress may therefore alter the balance within the follicle. Genetics can also influence sebaceous gland size, sebum composition, and the tendency toward follicular blockage. Some individuals naturally produce thicker or more lipid-dense sebum, which may contribute to persistent blackheads and clogged pores.
External factors further shape the microenvironment of pores. Heavy or occlusive skincare products may trap oil and debris on the skin surface, increasing the likelihood that pores become blocked. Inadequate cleansing routines can allow residue, sunscreen, and environmental particles to accumulate within follicles. Conversely, overly harsh skincare practices may damage the skin barrier, triggering increased oil production as the skin attempts to compensate. Environmental conditions such as heat, humidity, and friction from clothing or masks may also contribute to localized pore congestion in acne-prone individuals.
Understanding the internal conditions of acne-prone pores helps explain why certain skincare ingredients are commonly recommended. Salicylic acid is widely used because it is oil-soluble and can penetrate into the pore to help dissolve accumulated sebum and loosen compacted dead skin cells. Topical retinoids are often recommended in dermatology because they help normalize follicular keratinization, reducing the formation of new comedones over time. Benzoyl peroxide may help reduce bacterial populations within clogged follicles and decrease inflammatory activity associated with acne lesions. Ingredients such as niacinamide are frequently included in skincare formulations because they may help regulate oil production and support the skin barrier.
Consistent skincare practices often play an important role in maintaining a healthier pore environment. Gentle cleansing, appropriate exfoliation, and the use of non-comedogenic products may help limit the buildup of pore-clogging material. However, acne development is influenced by multiple biological factors, and improvement typically occurs gradually rather than immediately. Even well-designed routines may require several weeks to show noticeable changes in pore congestion and breakout frequency.
Because acne can vary significantly in severity and underlying causes, professional guidance may be beneficial for persistent or severe cases. Dermatologists can evaluate the skin’s condition and recommend prescription treatments, procedural options, or personalized skincare strategies when necessary. Understanding the complex microenvironment inside acne-prone pores helps explain why acne management often requires a combination of approaches that address oil production, follicular keratinization, bacterial balance, and inflammation simultaneously.