Video 1
Video 2
Video 3
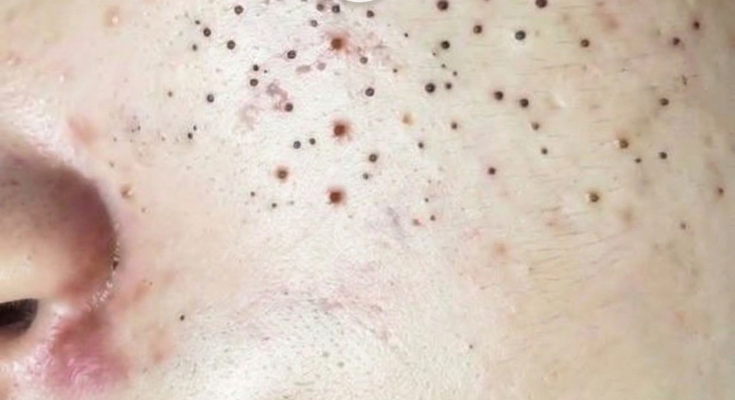
Pores become chronically clogged when the normal cycle of skin cell turnover and oil flow inside the hair follicle becomes persistently disrupted. Each pore contains a sebaceous gland that produces sebum, an oily substance that helps maintain skin hydration and barrier protection. Under typical conditions, sebum travels up the follicular canal and spreads across the skin surface. At the same time, dead skin cells shed gradually from the lining of the follicle. When these two processes remain balanced, pores stay relatively clear. However, when excess sebum combines with sticky keratinized skin cells, the material can accumulate inside the follicle and form a plug known as a comedone. Over time, repeated cycles of accumulation may cause certain pores to remain clogged for extended periods.
One of the central biological factors behind chronic pore congestion is a process called follicular keratinization. In acne-prone skin, cells within the follicle may shed more rapidly and adhere together instead of separating normally. This creates a dense mixture of keratin and oil that can become trapped within the pore opening. When the pore remains sealed, the plug may appear as a whitehead. If the surface opens and the contents oxidize when exposed to air, it can appear as a blackhead. The presence of the bacterium Cutibacterium acnes within the follicle can also contribute to local inflammation, further disrupting the normal structure of the pore and allowing blockages to persist.
Hormonal influences often play a significant role in why some individuals develop repeatedly clogged pores. Androgens, a group of hormones present in all sexes, stimulate sebaceous glands to produce more sebum. During periods of hormonal fluctuation such as puberty, menstrual cycles, or certain endocrine conditions, increased oil production can make it easier for keratin and sebum to accumulate within follicles. Genetic predisposition may also influence how strongly sebaceous glands respond to hormonal signals, which helps explain why some people experience persistent comedonal acne even with consistent skincare.
Skincare habits and cosmetic product choices may also influence whether pores become chronically congested. Heavy occlusive formulations, certain oils, or ingredients that trap dead skin cells against the follicular opening can contribute to blockage in susceptible individuals. Infrequent cleansing, aggressive scrubbing, or overuse of harsh products may further disrupt the skin barrier. When the barrier becomes irritated or inflamed, the follicle can respond by producing more oil and inflammatory mediators, which may worsen clogged pores over time.
Environmental factors can also influence pore congestion. Air pollution particles may adhere to sebum on the skin surface and accumulate around follicular openings. Humid climates can increase oiliness, while friction from tight clothing, helmets, or frequent touching of the face may mechanically block pores. Diet patterns that influence insulin signaling have also been studied for their potential role in stimulating sebaceous gland activity, though the relationship between diet and acne varies between individuals.
Consistent skincare strategies often aim to normalize the processes that lead to pore blockage. Ingredients such as salicylic acid are commonly used because they are oil-soluble and can penetrate into pores to help loosen accumulated keratin and sebum. Topical retinoids are widely recommended in dermatology because they regulate skin cell turnover and may help prevent the formation of new comedones. Benzoyl peroxide may help reduce populations of Cutibacterium acnes and decrease inflammatory activity within the follicle. Niacinamide is frequently included in formulations for oily or acne-prone skin because it may help support the skin barrier while moderating sebum production.
Gentle cleansing routines, non-comedogenic moisturizers, and consistent use of sunscreen may help support overall skin balance and prevent additional irritation that could worsen clogged pores. Professional dermatologic treatments such as prescription retinoids, chemical exfoliation, or manual comedone extraction may be considered when persistent pore congestion does not respond to over-the-counter approaches.
Because the biological tendencies that contribute to clogged pores often involve genetics and hormonal signaling, treatment typically focuses on long-term management rather than permanent elimination. Improvements often develop gradually as the skin cycle normalizes over several weeks or months. Individuals experiencing persistent or severe acne may benefit from consulting a qualified dermatologist who can evaluate underlying causes and recommend a treatment plan tailored to their skin type and medical history.