Taking notes is something most people do almost every day, whether in school, at work, or while learning a new skill.
Yet many of us have experienced the frustration of looking back at our notes and feeling confused.
Words are scattered across the page, key ideas are hard to find, and everything feels overwhelming.
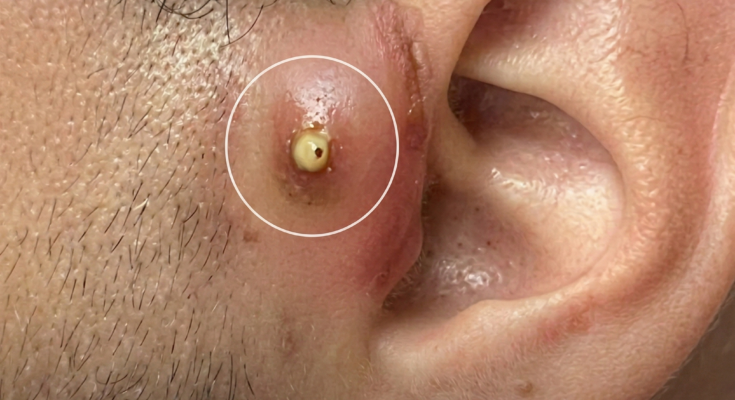
Mask-related acne, often referred to as acne mechanica, develops through a combination of mechanical friction, heat, occlusion, and altered skin microenvironment beneath the mask. When fabric rests tightly against the skin for prolonged periods, it increases friction along areas such as the cheeks, chin, and jawline. This friction can disrupt the skin barrier and stimulate inflammation within the follicle. At the same time, trapped heat and humidity create a microclimate that softens the stratum corneum and promotes swelling of keratinocytes inside the pore. This swelling can narrow the follicular opening and contribute to follicular keratinization, allowing sebum and dead skin cells to accumulate. The result may be clogged pores, blackheads, whiteheads, and inflammatory acne lesions in areas directly covered by the mask.
Sebum production continues throughout the day, and in individuals with oily skin or acne-prone skin, sebaceous glands may already be more active due to androgen influence. When masks limit airflow, sebum mixes with sweat and environmental debris, increasing the likelihood of comedone formation. Occlusive makeup or heavy skincare products worn under a mask can further trap oil and keratin within pores. Repeated mask use without adequate cleansing of reusable fabrics may also expose skin to residual bacteria and irritants. In some individuals, disruption of the skin microbiome combined with mechanical stress can amplify inflammation, leading to persistent breakouts even after individual pimples resolve.
Environmental and behavioral factors also play a role. Long work shifts, humid climates, and frequent speaking can increase moisture accumulation beneath masks. Over-cleansing in response to breakouts may weaken the skin barrier, leading to irritation-induced acne that resembles traditional inflammatory lesions. Conversely, insufficient cleansing may allow excess sebum and debris to remain inside follicles. Genetic predisposition to acne, baseline oil production, and sensitivity to friction all influence how severely someone experiences mask-related pore congestion.
Management strategies focus on reducing friction, minimizing occlusion, and supporting normal follicular turnover. Gentle cleansing twice daily with a mild, non-stripping cleanser helps remove sweat, oil, and debris without compromising barrier function. Salicylic acid is commonly used because it is oil-soluble and can penetrate into the pore lining to help dissolve accumulated keratin and sebum. Topical retinoids may help normalize follicular keratinization and reduce the formation of microcomedones, the earliest stage of acne. Benzoyl peroxide can reduce Cutibacterium acnes proliferation and may be considered for inflammatory lesions, although lower concentrations are often better tolerated under occlusive conditions. Niacinamide may help regulate oil production and support barrier repair while reducing visible redness.
Selecting lightweight, non-comedogenic skincare products can reduce additional occlusion under the mask. Avoiding heavy foundations during prolonged mask wear may decrease congestion, and using breathable, well-fitting masks made from soft materials can reduce mechanical irritation. Reusable masks should be washed regularly with fragrance-free detergents to minimize contact irritation. For individuals experiencing persistent or worsening acne, dermatologic treatments such as prescription retinoids, topical antibiotics, or short courses of anti-inflammatory medications may be recommended under medical supervision.
Improvement typically requires several weeks because acne develops at the level of the follicle before becoming visible on the surface. Consistency and gradual adjustments are important to avoid triggering additional irritation. While mask-related acne can be frustrating, it is generally manageable with evidence-based skincare and attention to barrier health. Individuals with severe, scarring, or treatment-resistant acne should consult a qualified dermatologist for personalized evaluation and care. This educational content follows established dermatology-based principles for acne and pore management.