Many of us have had moments in our lives when math seemed like an abstract concept, one that belonged in a classroom rather than in the real world.
The truth is, math is woven into the fabric of our daily lives more than we often realize.
From budgeting our finances to cooking a meal, the principles of mathematics quietly guide us through many everyday situations.
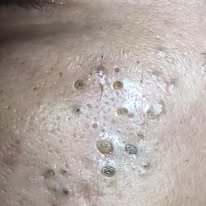
Closed and open comedones are non-inflammatory acne lesions that develop from the same underlying biological process: follicular keratinization combined with excess sebum production. Within each pore, or pilosebaceous unit, skin cells naturally shed and rise to the surface. When this shedding process becomes irregular, dead skin cells can accumulate inside the follicle. At the same time, sebaceous glands may produce increased amounts of oil, particularly in individuals with oily skin or during periods of hormonal fluctuation. The mixture of retained keratinocytes and sebum forms a plug, creating what is known as a comedo.
A closed comedo, commonly referred to as a whitehead, forms when the follicular opening remains covered by a thin layer of skin. Because the pore opening is blocked, the trapped material is not exposed to air. This results in a small, flesh-colored or white bump beneath the skin surface. In contrast, an open comedo, known as a blackhead, occurs when the pore remains partially open. The contents of the clogged pore are exposed to oxygen, leading to oxidation of melanin and lipids within the debris. This oxidation process, not dirt, gives blackheads their characteristic dark appearance. Both lesion types are considered non-inflammatory, but they can progress to inflamed papules or pustules if bacterial overgrowth and immune activation occur.
Several contributing factors influence whether someone develops closed or open comedones. Hormonal changes, particularly increases in androgens during adolescence or adulthood, can stimulate sebum production and make pores more prone to clogging. Genetic predisposition may affect sebaceous gland activity and the rate of skin cell turnover. Environmental influences such as humidity, occlusive cosmetics, or heavy skincare products may further contribute to blocked pores. Inconsistent cleansing habits or overuse of harsh exfoliants can also disrupt the skin barrier. When the barrier becomes compromised, irritation and compensatory oil production may worsen comedonal acne rather than improve it.
Effective management focuses on normalizing pore function and reducing excess oil without damaging the skin barrier. Topical retinoids are often recommended because they help regulate keratinocyte turnover inside the follicle, reducing the formation of new comedones. Over-the-counter retinoid formulations may help with mild comedonal acne, while prescription-strength options are commonly used for more persistent cases. Salicylic acid, a beta hydroxy acid that is oil-soluble, can penetrate into pores and assist in dissolving debris, making it particularly useful for blackheads. Benzoyl peroxide is primarily used for inflammatory acne due to its antibacterial properties, but it may be incorporated when mixed lesions are present. Niacinamide may help regulate oil production and support the skin barrier, making it a supportive ingredient in acne-focused skincare routines.
Gentle cleansing with a non-comedogenic formulation may help remove surface oil and impurities without stripping the skin. Over-exfoliation, aggressive scrubbing, or frequent pore extraction can irritate the follicle and potentially worsen breakouts. Professional treatments such as chemical peels or comedone extraction performed by trained dermatology providers may be considered for individuals with persistent clogged pores. In moderate to severe cases, dermatologists may recommend combination therapy to address both comedonal and inflammatory components of acne.
Realistic expectations are important when treating closed and open comedones. Because acne develops from processes occurring deep within the pore, visible improvement often takes several weeks. Consistency and patience are typically required, especially when using retinoids, which may initially cause mild dryness or irritation. Individuals with ongoing or severe acne should consult a qualified healthcare professional for personalized evaluation and treatment guidance. While both blackheads and whiteheads are common and manageable, safe, evidence-informed care helps reduce the risk of scarring and supports long-term skin health.