In a world where information flows endlessly, the joy of reading can sometimes feel fleeting.
Many of us have experienced that moment when we close a book, only to realize that the details have slipped away like sand through our fingers.
If you’ve ever wondered how to make reading stick in your mind, you’re not alone.
Dead skin cell buildup within the hair follicle is a central event in the development of comedones, the non-inflammatory lesions commonly recognized as blackheads and whiteheads. Under normal conditions, keratinocytes lining the follicular wall mature and shed in a controlled, microscopic process that allows sebum to move freely to the skin’s surface. In acne-prone skin, this desquamation process becomes disrupted. Keratinocytes may proliferate more rapidly and adhere to one another instead of separating efficiently. As these cells accumulate within the pore, they combine with sebum to form a dense plug. This early obstruction, known as a microcomedone, represents the first stage of acne lesion development and can evolve into visible comedones over time.
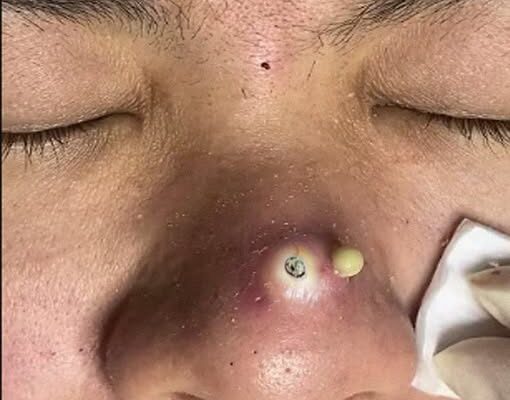
When dead skin cells and oil collect within the follicle, the structure of the pore begins to change. If the follicular opening remains relatively open, the trapped material is exposed to air and undergoes oxidation, leading to the dark appearance characteristic of blackheads. If the opening is narrower or fully blocked, the material remains beneath the surface, forming a whitehead. Both types of comedones originate from the same biological process of abnormal follicular keratinization combined with excess sebum production. This buildup also creates an environment where Cutibacterium acnes can proliferate, which may contribute to inflammation and the progression from non-inflammatory clogged pores to red, inflamed acne lesions.
Multiple factors can influence dead skin cell accumulation inside pores. Hormonal fluctuations, particularly increased androgen activity, stimulate sebaceous glands and increase oil output. Higher levels of sebum can make retained keratinocytes more likely to clump together and form plugs. Genetic predisposition may affect how cohesive follicular cells are or how reactive the skin is to hormonal signals. Environmental factors, including humidity and occlusive skincare products, may further contribute to pore congestion. In some cases, aggressive cleansing or over-exfoliation disrupts the skin barrier, leading to irritation that can worsen abnormal shedding patterns rather than improve them.
Effective management strategies often focus on normalizing cell turnover and reducing excess oil. Topical retinoids are commonly recommended because they help regulate keratinocyte behavior within the follicle and reduce microcomedone formation. With consistent use, they may decrease the number of blackheads and whiteheads while improving overall skin texture. Salicylic acid is frequently used in formulations for oily skin because it is oil-soluble and can penetrate into the pore lining, assisting with exfoliation of accumulated dead cells. Benzoyl peroxide primarily targets acne-causing bacteria and inflammation but may also help prevent clogged pores from progressing into inflamed lesions. Niacinamide is often incorporated to support the skin barrier and assist with oil regulation, complementing other active ingredients.
Because comedones form gradually beneath the surface, visible improvements typically require several weeks of consistent skincare. Overly harsh or rapid treatment approaches can irritate the skin and compromise barrier function, potentially worsening congestion. Individuals with persistent, widespread, or scarring acne may benefit from consultation with a qualified dermatologist, who can recommend prescription-strength retinoids or combination therapies tailored to individual skin type and acne severity. Understanding how dead skin cell buildup contributes to comedone formation underscores the importance of balanced, evidence-informed skincare aimed at maintaining healthy follicular turnover and long-term pore clarity.