In the bustling world of entrepreneurship, the journey of launching a startup can feel both exhilarating and daunting.
At the heart of every successful venture lies a well-crafted strategy, a roadmap that guides founders through the myriad of decisions and challenges they will face.
Exploring the basics of startup strategy can provide clarity and direction, helping aspiring entrepreneurs navigate their way toward success.
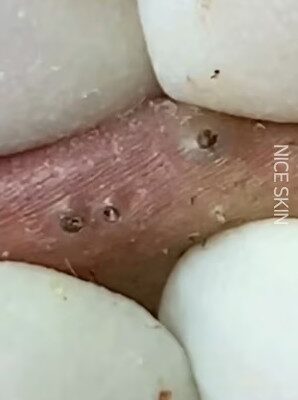
Comedonal acne develops when pores become obstructed by a combination of excess sebum and abnormal shedding of skin cells within the hair follicle. Each pore contains a sebaceous gland that produces oil to lubricate and protect the skin. In acne-prone individuals, sebum production may increase under hormonal influence, particularly androgens. At the same time, the lining of the follicle can undergo altered keratinization, meaning dead skin cells do not shed evenly. Instead of rising to the surface and dispersing, these cells mix with sebum and accumulate inside the pore. This process forms a microcomedone, the earliest invisible stage of acne. As the blockage enlarges, it becomes visible as either an open comedone, commonly known as a blackhead, or a closed comedone, often referred to as a whitehead.
The difference between blackheads and whiteheads is related to how the pore opening behaves. In blackheads, the follicular opening remains partially open, and the material inside is exposed to air. Oxidation of melanin and lipids causes the dark appearance, rather than dirt. In whiteheads, the pore opening remains closed, trapping the contents beneath the skin surface. Both forms are considered non-inflammatory acne, yet they can progress to inflamed lesions if bacteria proliferate and the follicle wall ruptures. Understanding this biological mechanism is important because comedonal acne is primarily driven by clogged pores rather than infection alone.
Several factors can contribute to pore congestion. Hormonal fluctuations during adolescence, menstrual cycles, pregnancy, or conditions involving androgen excess may increase oil production and predispose individuals to oily skin and blackheads. Genetic factors influence pore size, sebum output, and inflammatory tendencies. Skincare habits also play a significant role. Heavy or occlusive cosmetic products may contribute to pore blockage in susceptible individuals, particularly if they are not thoroughly removed. Inadequate cleansing, aggressive scrubbing, or overuse of harsh products can disrupt the skin barrier, potentially triggering compensatory oil production and worsening comedones. Environmental elements such as humidity, pollution, and friction from masks or helmets may further aggravate clogged pores.
Evidence-informed treatment for comedonal acne focuses on normalizing follicular turnover and reducing excess oil while protecting the skin barrier. Topical retinoids are commonly recommended because they help regulate keratinization and promote more orderly shedding of skin cells within the follicle. By preventing the formation of new microcomedones, retinoids address the underlying mechanism of blackheads and whiteheads. Salicylic acid, a beta hydroxy acid, is oil-soluble and can penetrate into pores to help dissolve accumulated debris. It may be particularly beneficial for individuals with oily skin and visible congestion. Benzoyl peroxide is more frequently used for inflammatory acne due to its antibacterial properties, but it can sometimes be combined with other treatments when mixed acne types are present.
Supportive ingredients such as niacinamide may help regulate sebum production and support barrier function, which is important when using active treatments that can cause dryness or irritation. Gentle cleansing with non-comedogenic formulations is often advised, along with moisturizers that maintain hydration without occluding pores. Overly aggressive exfoliation or frequent use of multiple strong actives can increase irritation and paradoxically worsen breakouts.
For persistent or widespread comedonal acne, dermatology-based options may include prescription-strength retinoids, combination topical therapies, hormonal treatments in appropriate patients, or in-office procedures such as professional comedone extraction or chemical peels. These interventions should be tailored to individual skin type, acne severity, and tolerance. Because acne is a chronic condition influenced by multiple internal and external factors, improvement typically occurs gradually over several weeks to months rather than immediately.
Realistic expectations are essential. Even well-formulated skincare ingredients require consistent use to show measurable change, and temporary irritation or mild purging may occur when beginning retinoid therapy. While many people achieve significant reduction in clogged pores and whiteheads with appropriate treatment, ongoing maintenance is often necessary. Individuals experiencing severe, scarring, or treatment-resistant acne are encouraged to consult a qualified dermatologist to develop a personalized plan.