Life is a journey filled with twists and turns, and for many, the path to success is often paved with challenges.
This is particularly true for famous authors who have faced adversity in their lives.
Their stories are not just about the books they wrote but also about the obstacles they overcame to share their voices with the world.
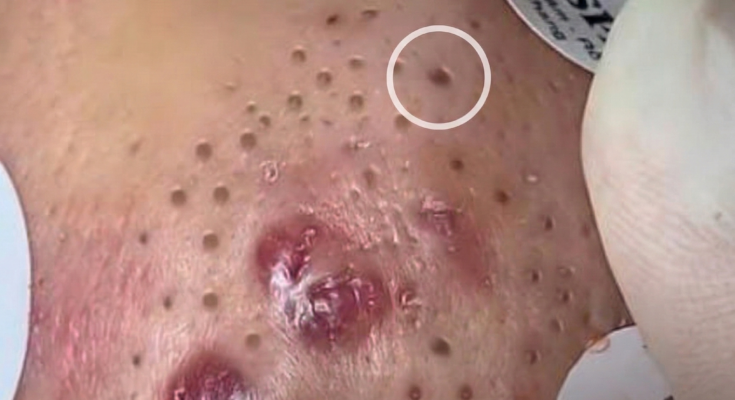
Acne often begins long before any visible blemish appears on the skin. The earliest stage of acne development involves the formation of microscopic blockages inside hair follicles known as microcomedones. These structures are too small to be seen with the naked eye, yet they represent the biological starting point of both blackheads and whiteheads. Microcomedones develop when the normal process of skin cell turnover inside the follicle becomes disrupted, allowing dead keratinocytes to accumulate and mix with sebum produced by nearby sebaceous glands. This combination forms a sticky plug that gradually obstructs the follicular opening.
Under healthy conditions, skin cells lining the follicle shed in a controlled pattern and are carried out of the pore with sebum. In acne-prone skin, however, a process called follicular keratinization becomes irregular. Cells may shed more rapidly or adhere together more strongly than normal, making them less likely to exit the follicle efficiently. As this buildup continues, the mixture of dead cells and oil forms a compact structure that remains trapped beneath the skin surface. At this early stage, the pore may appear normal from the outside even though the internal blockage is already forming.
Sebum production plays a major role in the progression of microcomedones. Sebaceous glands attached to hair follicles produce lipids that help maintain skin hydration and barrier function. When sebum production increases, which is common during hormonal fluctuations such as puberty, menstrual cycles, or periods of elevated androgen activity, the excess oil can further contribute to follicular blockage. The oily environment within the pore also creates conditions that may support the proliferation of Cutibacterium acnes, a bacterium associated with inflammatory acne.
Several external and internal factors can influence how frequently microcomedones develop. Genetic predisposition affects sebaceous gland size and oil production levels, making some individuals more prone to clogged pores. Certain cosmetic or skincare products that are highly occlusive may contribute to follicular blockage in susceptible skin. Environmental factors such as humidity, sweat, and friction from clothing or masks can also increase the likelihood of pore congestion. In addition, aggressive cleansing or overly drying treatments may disrupt the skin barrier, which sometimes triggers compensatory oil production that further complicates acne-prone skin.
Over time, microcomedones can evolve into visible acne lesions. If the follicular opening remains closed, the trapped material forms a whitehead, also known as a closed comedone. If the pore opening widens and the contents are exposed to air, oxidation of lipids and melanin can cause the dark appearance characteristic of blackheads. In some cases, bacterial activity and immune responses lead to inflammation, resulting in papules, pustules, or deeper acne lesions.
Skincare strategies aimed at preventing acne often focus on interrupting microcomedone formation before visible breakouts occur. Topical retinoids are commonly recommended because they help normalize follicular keratinization and promote more regular shedding of skin cells inside pores. Salicylic acid, a beta hydroxy acid that penetrates oily follicles, may assist in dissolving accumulated debris and reducing pore congestion. Benzoyl peroxide is frequently used to reduce acne-associated bacteria, while ingredients such as niacinamide may help support oil regulation and calm inflammation in acne-prone skin.
Consistency is important because the microcomedone stage can develop weeks before a breakout becomes visible. This delay often explains why acne treatments may take several weeks to show noticeable improvement. Dermatologists typically advise maintaining a regular skincare routine and allowing sufficient time for active ingredients to influence the follicular cycle.
Although many over-the-counter treatments can help manage early pore clogging, persistent or severe acne may require evaluation by a qualified healthcare professional. Dermatologists can recommend prescription treatments, adjust skincare routines, and address underlying hormonal or inflammatory factors when necessary. Understanding the hidden microcomedone stage highlights why long-term pore maintenance is often essential for managing acne-prone skin and reducing the frequency of future breakouts.