In our fast-paced digital world, the way we communicate online can often feel overwhelming.
Social media platforms, blogs, and forums are brimming with opinions, images, and narratives that compete for our attention.
Amidst this cacophony, practicing mindful posting can be a refreshing approach that not only enhances your online experience but also contributes positively to the digital community.
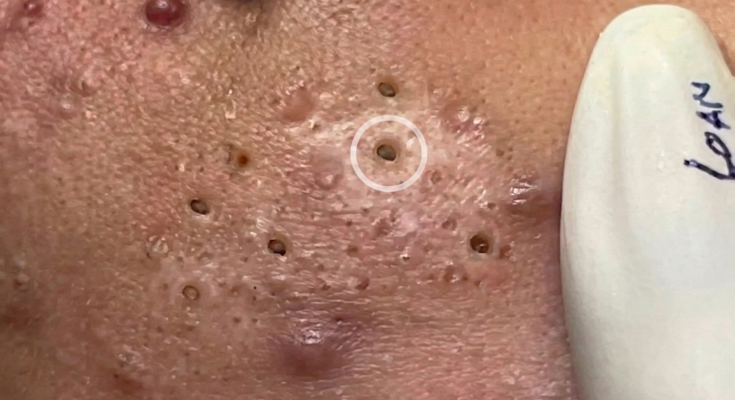
Acne often begins with subtle changes inside the hair follicle, particularly in individuals with oily or acne-prone skin. Each pore contains a hair follicle lined with keratinocytes, which are skin cells that normally grow, mature, and shed in a controlled cycle. Under healthy conditions, these dead skin cells are gradually released from the follicular lining and carried to the surface along with sebum, the oil produced by sebaceous glands. In acne-prone follicles, however, this shedding process becomes disrupted. Instead of separating cleanly, the cells tend to stick together and accumulate inside the pore, forming a dense mixture with sebum that can block the follicular opening. This process, known as follicular keratinization, is considered one of the earliest biological steps in comedone formation and plays a central role in the development of blackheads and whiteheads.
Several biological factors can increase the likelihood of this buildup. Hormonal influences are among the most significant. Androgens stimulate sebaceous glands to produce more oil, particularly during adolescence, menstrual cycles, or periods of hormonal fluctuation. When excess sebum fills the follicle, it mixes with keratinized cells and slows their natural exit from the pore. This oily environment can make the follicle more adhesive internally, encouraging dead cells to clump together rather than shed individually. As the material accumulates, it gradually forms a microscopic plug that may later develop into a visible comedone.
Genetic predisposition also plays an important role in how follicles handle dead skin cell turnover. Some individuals naturally produce larger sebaceous glands or have follicles that generate keratinocytes more rapidly. In these cases, the rate of cell production may exceed the rate at which cells are removed from the pore. Over time, repeated cycles of incomplete shedding can lead to chronic pore congestion. Environmental factors may further contribute to this process. Heat, humidity, occlusive cosmetics, and heavy skincare products can increase oil retention and reduce normal follicular ventilation, creating conditions that favor dead cell accumulation.
Skincare habits may also influence how efficiently dead skin cells are removed from acne-prone pores. Inadequate cleansing can allow oil, cosmetic residue, and environmental particles to combine with keratinized cells inside the follicle. Conversely, overly aggressive cleansing or harsh scrubbing may disrupt the skin barrier and trigger compensatory oil production, which can worsen congestion in some individuals. Products that clog pores or create heavy occlusion may further slow the natural release of follicular debris.
Because dead skin cell accumulation is a core mechanism in acne development, many acne treatments are designed to normalize this process. Topical retinoids are widely used in dermatology because they help regulate keratinocyte turnover and reduce the tendency for cells to stick together inside follicles. By promoting more organized shedding of skin cells, retinoids may help keep pores clearer over time. Beta hydroxy acids such as salicylic acid are also commonly recommended because they are oil-soluble and can penetrate into the pore lining, where they help loosen compacted debris and support exfoliation within the follicle.
Other ingredients may support the overall environment of acne-prone skin. Benzoyl peroxide is often used to reduce bacterial activity associated with inflammatory acne lesions, while niacinamide may help regulate oil production and support the skin barrier. Consistent use of non-comedogenic moisturizers and sunscreens can also help maintain barrier balance without contributing to pore blockage.
It is important to recognize that the process of follicular cell buildup develops gradually, often over weeks before visible acne appears. For this reason, treatments designed to regulate cell turnover and maintain clear pores typically require consistent use over time. Improvements may occur gradually as the follicular environment stabilizes and the cycle of congestion becomes less frequent.
Persistent or severe acne may require evaluation by a dermatologist, who can determine whether prescription treatments, hormonal therapies, or procedural options are appropriate. With appropriate management and consistent skincare practices, many individuals are able to reduce the accumulation of dead skin cells within pores and improve long-term control of acne-prone skin.