In our everyday lives, we often encounter situations that remind us of the delicate dance between temperature and physical matter.
Have you ever noticed that a metal lid can be particularly stubborn to open after a meal? Or perhaps you’ve felt the smoothness of a wooden chair becoming less inviting on a hot summer day? These seemingly simple experiences are reflections of a fascinating phenomenon known as thermal expansion.
Thermal expansion is the tendency of matter to change its shape, area, and volume in response to a change in temperature.
Follicular keratinization is one of the central biological processes involved in the development of acne lesions. The inner lining of the hair follicle is composed of keratinocytes, which are specialized skin cells responsible for producing keratin and forming part of the protective outer layer of the skin. Under normal conditions, these cells grow, mature, and shed in an organized cycle that allows them to exit the follicle along with sebum. When this process functions efficiently, pores remain relatively clear and oil flows smoothly to the surface of the skin. However, in acne-prone skin the process of keratinization may become disrupted, leading to the accumulation of dead skin cells inside the follicle.
When keratinocytes begin to shed irregularly, they may stick together rather than separating and exiting the pore individually. This increased cohesion causes layers of cells to accumulate within the follicular canal. At the same time, sebaceous glands continue to produce sebum, which mixes with the retained keratinocytes and forms a dense plug. This early blockage is known as a microcomedone and represents the initial stage of acne lesion development, even before visible blackheads or whiteheads appear on the skin surface.
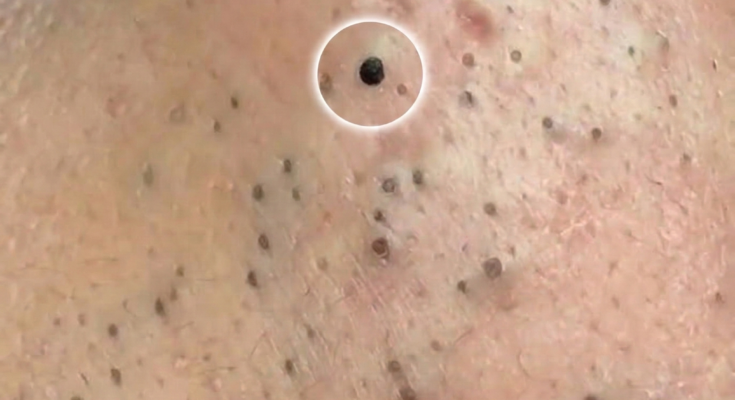
As the blockage grows, it gradually expands the pore and begins to alter the environment inside the follicle. When the follicular opening remains partially open, the accumulated material may be exposed to oxygen, which can darken the surface of the plug and form a blackhead. If the follicular opening becomes sealed beneath the skin, the trapped material forms a whitehead. Both of these lesions are considered non-inflammatory forms of acne, but they create conditions that may later lead to inflammation.
The buildup of keratinocytes and sebum also creates an environment where Cutibacterium acnes bacteria can multiply more easily. These bacteria naturally live on the skin, but when trapped inside a blocked follicle they may contribute to the production of inflammatory mediators. The immune system may then respond by sending inflammatory cells to the area, leading to redness, swelling, and the formation of papules, pustules, or deeper nodular lesions.
Several factors can influence how strongly follicular keratinization contributes to acne. Hormonal signals, particularly androgens, may increase sebum production and indirectly worsen pore blockage. Genetic predisposition can also play a role in how follicles regulate cell turnover. Certain skincare habits, including the use of heavy or occlusive cosmetic products, may further slow the natural clearance of pores in some individuals. Environmental factors such as humidity, pollution, and prolonged skin occlusion may also affect how easily debris accumulates inside follicles.
Many evidence-based acne treatments aim to normalize the process of follicular keratinization. Topical retinoids are widely used because they help regulate keratinocyte turnover and reduce the formation of microcomedones over time. Salicylic acid is another commonly used ingredient because it can penetrate oily follicles and assist in loosening accumulated debris inside pores. Benzoyl peroxide may be introduced when inflammatory lesions develop, as it helps reduce acne-associated bacteria and inflammatory activity within the follicle. Niacinamide is often included in supportive skincare routines because it may help regulate oil production while supporting the skin barrier.
Improvements in acne related to follicular keratinization often require patience because the skin renews itself gradually over several weeks. Consistent use of appropriate skincare ingredients may help reduce the formation of new clogged pores, but results typically develop over time rather than immediately. Individuals experiencing persistent, widespread, or scarring acne may benefit from consultation with a qualified dermatologist, who can assess the severity of the condition and recommend treatments tailored to the underlying causes of follicular blockage and inflammation.