In a world that often feels fast-paced and demanding, the journey of self-discovery can sometimes seem daunting.
Yet, there lies a gentle yet powerful approach to uncovering our strengths: open learning.
This method invites us to explore our interests and abilities in a way that feels natural and fulfilling, allowing us to grow and thrive in our own unique ways.
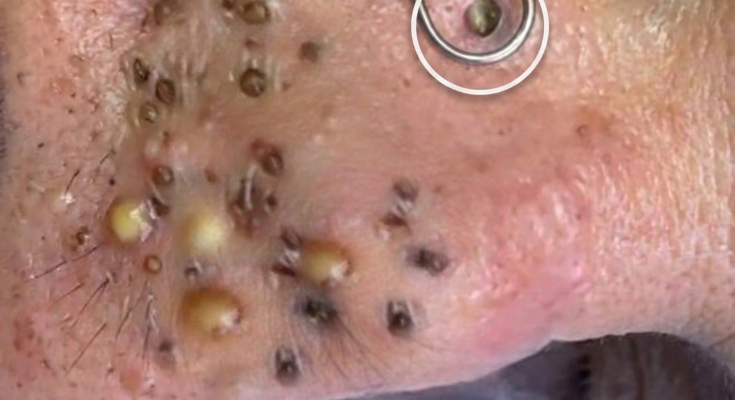
The early stages of comedone formation begin deep within the pilosebaceous unit, a structure composed of a hair follicle and its associated sebaceous gland. In acne-prone skin, this environment can become favorable for the development of microscopic blockages long before visible blemishes appear. The process typically starts with changes in the way keratinocytes, the skin cells lining the follicle, shed and renew themselves. Instead of separating and exiting the pore normally, these cells may accumulate and mix with sebum, the oily substance produced by sebaceous glands. This combination forms a sticky material that gradually narrows the follicular opening and begins the earliest stage of a clogged pore.
Sebum production plays an important role in this process. Sebaceous glands respond to hormonal signals, particularly androgens, which can increase oil output during adolescence and other hormonal shifts. When excess sebum is present in the follicle, it can combine with retained keratinocytes to create a dense mixture known as a microcomedone. At this stage the blockage is microscopic and cannot yet be seen on the skin surface, but it represents the starting point from which blackheads, whiteheads, and inflammatory acne lesions may eventually develop.
Changes in follicular keratinization are considered one of the central biological mechanisms behind early comedone formation. In acne-prone individuals, the turnover of cells inside the follicle may become irregular, leading to increased cohesion between cells. Instead of shedding individually, keratinocytes cluster together and form compact plugs within the pore. Over time, these plugs can trap additional sebum and cellular debris, gradually expanding the obstruction and creating the conditions necessary for visible comedones to form.
Several contributing factors can influence how easily this early blockage develops. Hormonal fluctuations may stimulate greater sebaceous gland activity, increasing the amount of oil available to mix with dead skin cells. Genetic predisposition can also affect how follicles respond to hormonal signals and regulate cell turnover. Environmental factors such as humidity, occlusive skincare products, or heavy cosmetics may further contribute by creating conditions that slow normal pore clearance. In some individuals, the presence of Cutibacterium acnes bacteria inside the follicle can interact with trapped sebum, potentially triggering inflammatory responses as the blockage progresses.
Early intervention strategies often focus on maintaining normal follicular turnover and reducing the accumulation of excess oil. Topical retinoids are commonly recommended because they help normalize keratinocyte shedding and may reduce the formation of microcomedones. Ingredients such as salicylic acid are frequently used in acne skincare routines because they are oil-soluble and can penetrate into the pore, assisting with the exfoliation of accumulated debris. Benzoyl peroxide is often included when inflammatory acne develops, as it targets acne-associated bacteria, while niacinamide may help support oil regulation and calm visible redness in acne-prone skin.
Although these approaches may help reduce the formation of clogged pores over time, it is important to recognize that comedone formation is influenced by multiple biological factors that vary between individuals. Consistent skincare routines and gentle cleansing practices may support long-term pore maintenance, but improvements often occur gradually as the skin cycle renews itself. For individuals experiencing persistent or severe acne, evaluation by a dermatologist may help determine whether prescription treatments or additional therapies are appropriate to manage the underlying causes of comedone development.