The intricate dance between genes and behavior has fascinated scientists, psychologists, and curious minds alike.
As we navigate our daily lives, we often ponder the reasons behind our actions, reactions, and even our inclinations.
Are we merely products of our environment, shaped by our experiences? Or do our genes hold the key to understanding our behaviors? Exploring how genes influence behavior can deepen our understanding of ourselves and the world around us.
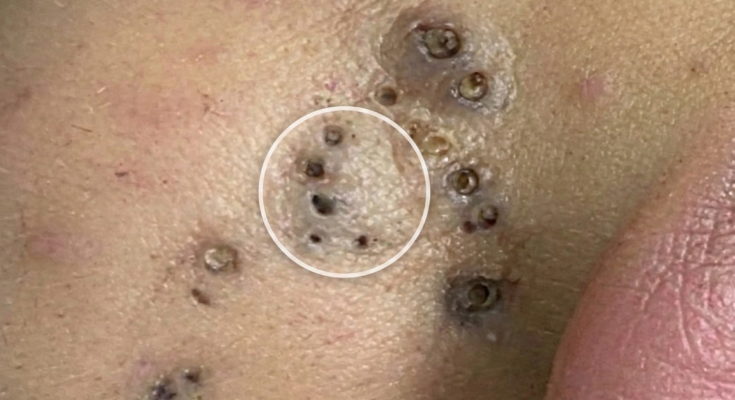
Purging and breakouts are often confused because both involve the sudden appearance of pimples, yet the biological processes behind them differ in important ways. Acne develops through a sequence that begins with increased sebum production, abnormal follicular keratinization, and the formation of microcomedones inside the pore. When these clogged pores remain trapped beneath the surface, they may later evolve into visible blackheads, whiteheads, or inflamed lesions. Purging occurs when a treatment accelerates this existing cycle, bringing underlying microcomedones to the surface more quickly. In contrast, a typical breakout forms when new pore blockages develop due to ongoing oil production, inflammation, bacterial proliferation, or barrier disruption.
Purging is most commonly associated with ingredients that increase skin cell turnover. Topical retinoids such as adapalene or tretinoin, chemical exfoliants like salicylic acid, and sometimes alpha hydroxy acids can stimulate faster desquamation within the follicle. As a result, preexisting clogged pores surface in a shorter timeframe than they would naturally. This can temporarily increase the appearance of acne lesions, particularly in areas where breakouts already tend to occur. Because the process reflects an acceleration of the comedonal life cycle rather than the creation of new blockages, purging typically appears in familiar acne-prone zones and begins within the first few weeks of starting a new active ingredient.
In contrast, regular breakouts are driven by factors that actively contribute to new pore obstruction and inflammation. Hormonal fluctuations can stimulate sebaceous glands to produce more oil, increasing the likelihood of clogged pores. Harsh skincare routines may impair the skin barrier, leading to irritation that worsens inflammatory acne. Occlusive or comedogenic products can trap sebum and dead skin cells within pores. Environmental stressors such as humidity and sweat may also contribute to congestion in individuals with oily skin. Unlike purging, breakouts may occur in new areas of the face or body and may persist or worsen without improvement over time.
The timeline and pattern of lesions can help distinguish between the two. Purging generally begins shortly after introducing an ingredient known to increase cell turnover and tends to stabilize within one to two skin cycles, often around four to eight weeks. The lesions are usually similar in type to prior acne, such as small whiteheads or blackheads in areas of preexisting comedonal acne. Breakouts, however, may develop at any time, especially after introducing a new product that clogs pores or irritates the skin. They may include more inflamed papules, pustules, or nodules and do not show gradual improvement with continued use of the product.
Management strategies differ accordingly. When purging is suspected, gradual introduction of retinoids or exfoliating acids can help minimize irritation while allowing the medication to normalize follicular keratinization over time. Supporting the skin barrier with non-comedogenic moisturizers containing ingredients such as niacinamide or ceramides may reduce excessive dryness and inflammation. Sunscreen use is also important, particularly when using retinoids or chemical exfoliants, as these ingredients can increase photosensitivity. If lesions are severe, painful, or persist beyond several weeks without improvement, reassessment by a dermatologist may be appropriate to determine whether the reaction represents irritation or true acne exacerbation.
When breakouts are the cause, adjusting the skincare routine may be necessary. Simplifying products, avoiding heavy occlusives, and selecting formulations labeled as non-comedogenic can reduce additional pore clogging. Evidence-based treatments such as benzoyl peroxide to target acne-causing bacteria or salicylic acid to penetrate oil within pores are commonly recommended for mild to moderate acne. In more persistent cases, prescription retinoids, topical antibiotics, hormonal therapies, or oral medications may be considered under medical supervision.
Understanding the difference between purging and breakouts can prevent premature discontinuation of beneficial treatments while also avoiding prolonged use of products that worsen acne. Both processes involve the biology of clogged pores, sebum production, and inflammation, but their triggers and trajectories differ. Realistic expectations are essential, as most acne treatments require consistent use over several weeks to show visible improvement. Individuals experiencing significant discomfort, widespread inflammation, or uncertainty about their skin’s response should consult a qualified healthcare professional for personalized guidance. This article follows evidence-based educational standards for acne and skincare content.