In the intricate tapestry of life on Earth, animals exhibit a stunning array of senses that allow them to interact with their surroundings in ways that often surpass human capabilities.
From the keen eyesight of an eagle soaring high above to the delicate olfactory senses of a bloodhound on the trail, the world of animal senses is a realm of wonder.
Understanding these senses not only enriches our appreciation for the animal kingdom but also sheds light on the evolutionary paths that have shaped these remarkable creatures.
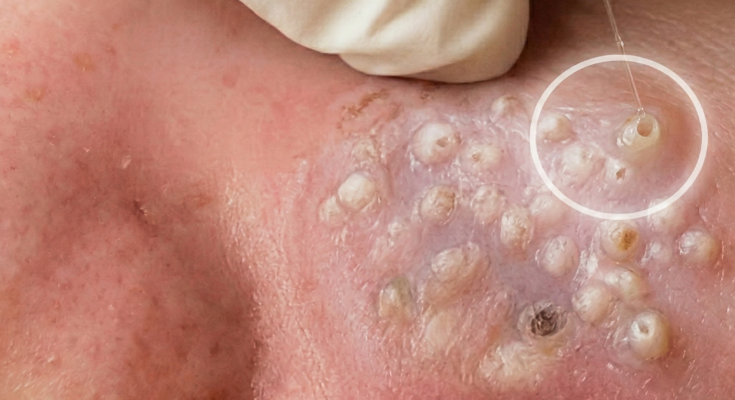
Acne develops within the pilosebaceous unit, where excess sebum production, abnormal follicular keratinization, and the accumulation of dead skin cells combine to clog pores. This environment supports the proliferation of Cutibacterium acnes, a bacterium naturally present on the skin. As bacterial byproducts and trapped debris build within the follicle, the immune system responds with inflammation, leading to papules, pustules, and in more severe cases, nodules. Topical antibiotics are used in acne care primarily to reduce bacterial overgrowth and calm inflammatory lesions, rather than to directly treat clogged pores such as blackheads and whiteheads.
Inflammatory acne is influenced by several factors, including hormonal fluctuations that increase oil production, genetic predisposition to heightened inflammatory responses, and skincare practices that may disrupt the skin barrier. Oily skin creates a lipid-rich environment that can support bacterial proliferation, while harsh cleansing or overwashing may weaken barrier function and worsen irritation. Environmental stressors and occlusive cosmetic products can further contribute to pore congestion. In this context, topical antibiotics are typically considered when red, inflamed breakouts persist despite appropriate use of non-antibiotic treatments.
Commonly prescribed topical antibiotics include clindamycin and erythromycin. These medications work by reducing the population of acne-associated bacteria and decreasing inflammatory signaling within the follicle. However, they do not normalize keratinization or directly dissolve excess sebum. For this reason, dermatology guidelines generally recommend that topical antibiotics be combined with other acne treatments that target different aspects of acne biology. Benzoyl peroxide is frequently paired with topical antibiotics because it has antibacterial properties and may help reduce the risk of bacterial resistance. Retinoids are often included in treatment plans because they help regulate cell turnover, prevent clogged pores, and improve comedonal acne. Ingredients such as salicylic acid may also support pore clearance, while niacinamide can help calm inflammation and support barrier repair.
Topical antibiotics are most often used for mild to moderate inflammatory acne rather than purely comedonal acne dominated by blackheads and whiteheads. They are typically prescribed for limited durations, as long-term or inappropriate use may contribute to antibiotic resistance. Resistance can reduce treatment effectiveness over time and has broader public health implications. For this reason, dermatologists generally avoid using topical antibiotics as standalone therapy and reassess treatment response regularly.
It is important to set realistic expectations. Improvement in inflammatory lesions may take several weeks, and consistent application as directed is necessary. Some individuals may experience mild dryness or irritation, particularly when topical antibiotics are combined with retinoids or benzoyl peroxide. Persistent, severe, or scarring acne warrants evaluation by a qualified healthcare professional, who may consider alternative therapies such as oral medications or procedural interventions. When used appropriately and as part of a comprehensive acne management plan, topical antibiotics can play a supportive role in reducing inflammation and helping restore clearer skin.