Reading comprehension is a skill that many of us take for granted.
Whether we’re diving into a thrilling novel, skimming an article online, or trying to grasp complex information for a project, understanding what we read is essential.
However, for some, reading comprehension can feel like a daunting task.
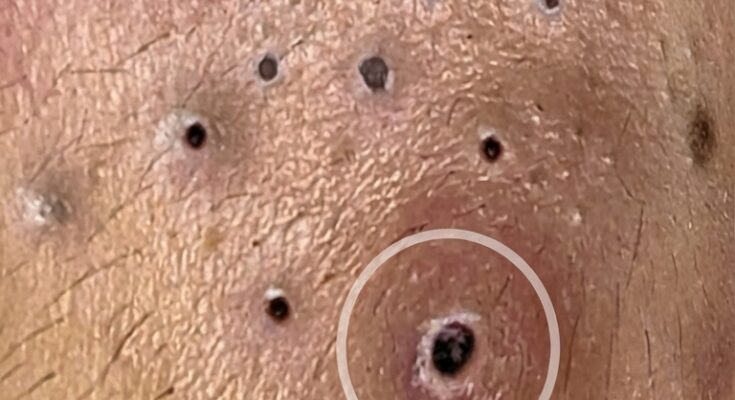
Post-inflammatory hyperpigmentation, often abbreviated as PIH, develops when inflammation within the skin triggers excess melanin production after an acne lesion heals. Acne is fundamentally an inflammatory disorder of the pilosebaceous unit, involving increased sebum production, abnormal follicular keratinization, clogged pores, and the formation of comedones such as blackheads and whiteheads. When the follicle becomes blocked and inflamed, immune cells release signaling molecules that stimulate melanocytes, the pigment-producing cells in the skin. As the breakout resolves, these melanocytes may deposit increased pigment in the affected area, leaving behind flat brown, red, or grayish marks that can persist long after the active acne has cleared.
The intensity and duration of post-inflammatory hyperpigmentation depend on the depth of inflammation and individual skin biology. Deeper inflammatory lesions, such as papules, pustules, or cystic acne, are more likely to disrupt the surrounding tissue and stimulate stronger pigment responses. Individuals with medium to deeper skin tones are biologically more prone to developing visible PIH because their melanocytes are more reactive to inflammatory signals. Repeated picking, squeezing, or aggressive exfoliation can further amplify inflammation and increase the likelihood of lingering discoloration. Environmental factors such as ultraviolet exposure also play a significant role, as UV radiation can darken existing pigmentation and prolong its persistence.
Although PIH is not the same as acne scarring, the two are often confused. True scars involve structural damage to collagen and may appear as depressions or raised areas. In contrast, post-inflammatory hyperpigmentation is a change in pigment without permanent structural alteration. This distinction is important because PIH can gradually fade over time, whereas scars often require procedural intervention. However, without appropriate skincare and sun protection, pigmentation may last for months or longer.
Effective management begins with controlling active acne to reduce ongoing inflammation. Ingredients such as salicylic acid may help by penetrating oil-filled pores and supporting the breakdown of excess keratin that contributes to clogged pores and comedonal acne. Benzoyl peroxide is commonly used to reduce bacterial overgrowth associated with inflammatory breakouts, which may indirectly lower the risk of post-inflammatory discoloration by limiting lesion severity. Topical retinoids, including over-the-counter retinol and prescription retinoids, are often recommended because they help normalize follicular keratinization, support cell turnover, and gradually improve uneven pigmentation. Consistent use over several months may contribute to visible fading.
Additional supportive ingredients can target pigment regulation and skin barrier function. Niacinamide is frequently included in formulations for acne-prone and oily skin because it may help regulate sebum production, calm inflammation, and reduce pigment transfer within the skin. Azelaic acid is another ingredient often recommended in dermatology settings, as it has both anti-inflammatory and pigment-modulating properties. Gentle chemical exfoliants such as alpha hydroxy acids can support surface cell turnover, but overuse may disrupt the barrier and worsen irritation, potentially prolonging hyperpigmentation.
Sun protection remains a central component of treatment. Broad-spectrum sunscreen helps prevent ultraviolet-induced darkening of existing marks and reduces new pigment stimulation. Even when acne is improving with retinoids or exfoliating skincare ingredients, unprotected sun exposure can counteract progress. Daily sunscreen use is often considered essential for managing PIH, particularly in individuals with darker skin tones who are more susceptible to persistent discoloration.
For persistent or extensive post-inflammatory hyperpigmentation, dermatologic procedures may be considered. Superficial chemical peels, prescription-strength retinoids, and certain laser or light-based treatments can be used selectively under professional supervision. These approaches require careful evaluation because aggressive treatments may worsen pigmentation in susceptible skin types if not appropriately selected and monitored.
Improvement in post-inflammatory hyperpigmentation is gradual. Epidermal pigmentation may fade over several months, while deeper dermal discoloration can take longer. Consistency, barrier-friendly skincare habits, and realistic expectations are important. Individuals experiencing ongoing breakouts, worsening discoloration, or uncertainty about treatment options are encouraged to consult a qualified dermatologist to develop a tailored plan that addresses both acne control and pigment management safely.