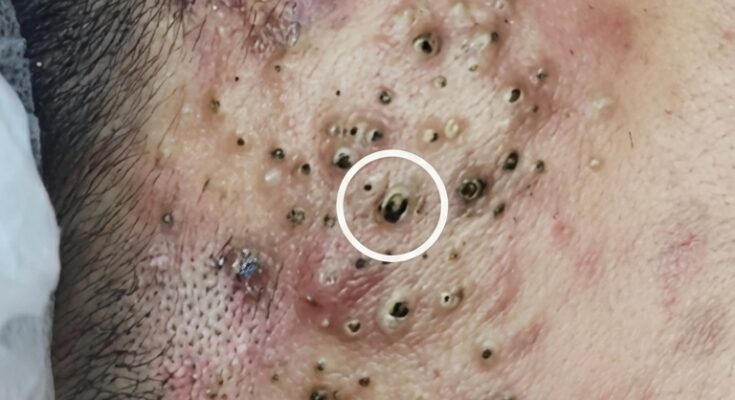
Acne in Adults: Why Breakouts Continue After Adolescence
Acne in adults develops through the same core biological mechanisms seen in adolescence, including increased sebum production, abnormal follicular keratinization, clogged pores, and inflammation. Microcomedones form when dead skin cells accumulate within the hair follicle and mix with sebum, creating an environment that can support the proliferation of Cutibacterium acnes. Although acne is commonly associated with puberty, these underlying processes can persist well beyond teenage years. In many adults, especially women, breakouts tend to concentrate along the lower face and jawline, reflecting hormonal influences on sebaceous gland activity.
Hormonal fluctuations remain one of the most significant contributors to adult acne. Androgens stimulate sebaceous glands, increasing oil production that can contribute to blackheads, whiteheads, and inflammatory lesions. Even when hormone levels fall within normal laboratory ranges, increased sensitivity of the oil glands may sustain breakouts. Menstrual cycle changes, pregnancy, perimenopause, and conditions such as polycystic ovary syndrome may influence acne patterns. Chronic stress can also elevate cortisol and indirectly affect oil production and inflammation. In addition, lifestyle factors including occlusive cosmetics, heavy moisturizers, frequent mask use, and environmental pollutants may contribute to clogged pores in adulthood.
Adult skin often presents additional complexity because barrier function tends to decline gradually with age. This can make skin more prone to irritation from strong acne treatments. Overuse of exfoliating acids, benzoyl peroxide, or harsh cleansers may disrupt the barrier, leading to dryness and compensatory oil production that can worsen acne. At the same time, slower cell turnover compared to adolescence may allow comedones to persist longer, making blackheads and clogged pores more noticeable. Genetic predisposition also plays a role, influencing sebaceous gland size, inflammatory response, and scarring risk.
Evidence-informed treatment for adult acne focuses on regulating cell turnover, controlling sebum, and minimizing inflammation while preserving barrier health. Topical retinoids are commonly recommended because they help normalize follicular keratinization and reduce the formation of new comedones. Salicylic acid may assist in clearing pore debris, particularly for oily skin types. Benzoyl peroxide can reduce bacterial overgrowth and is often used in combination regimens. Niacinamide may support barrier function and help reduce visible redness. For individuals with hormonally influenced acne, healthcare professionals may consider prescription options such as hormonal therapies or oral medications when appropriate.
Managing expectations is important. Adult acne can be chronic and may require ongoing maintenance rather than short-term treatment. Visible improvement typically takes several weeks, and inconsistent use of skincare ingredients may limit results. Because adult skin can be more sensitive, introducing active ingredients gradually and monitoring for irritation is advisable. Persistent, nodular, or scarring acne warrants evaluation by a qualified dermatologist to develop a personalized plan. Educational dermatology standards emphasize mechanism-based explanations and realistic guidance when addressing acne across the lifespan, supporting safe and sustainable management strategies.