In our everyday lives, we often encounter situations that remind us of the delicate dance between temperature and physical matter.
Have you ever noticed that a metal lid can be particularly stubborn to open after a meal? Or perhaps you’ve felt the smoothness of a wooden chair becoming less inviting on a hot summer day? These seemingly simple experiences are reflections of a fascinating phenomenon known as thermal expansion.
Thermal expansion is the tendency of matter to change its shape, area, and volume in response to a change in temperature.
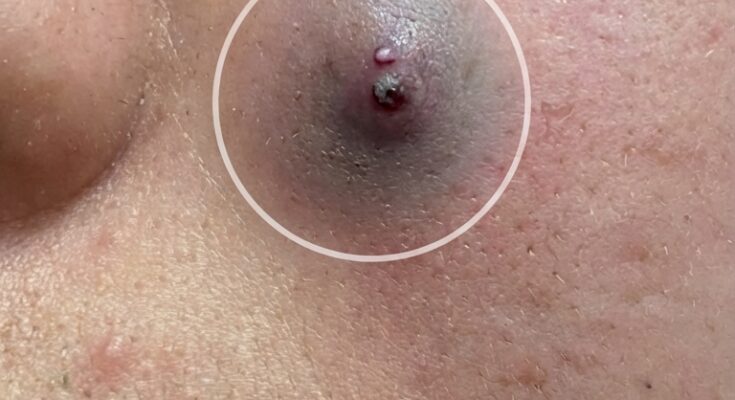
Acne begins long before a visible pimple forms on the surface of the skin. The earliest stage of a breakout is known as the microcomedone, a microscopic plug that develops inside the hair follicle. This process starts when keratinocytes, the cells that line the pore, begin to shed in an irregular pattern. Instead of dispersing normally, these cells accumulate and mix with sebum, the oily substance produced by sebaceous glands. As this mixture builds within the follicle, it creates a small blockage beneath the skin. At this stage, the lesion is invisible to the naked eye, yet it represents the true starting point of both inflammatory and non-inflammatory acne.
The formation of microcomedones is closely linked to changes in sebum production and follicular keratinization. During periods of hormonal fluctuation, particularly increases in androgens, sebaceous glands may produce more oil. Oily skin creates an environment in which dead skin cells are more likely to adhere together inside the pore. As the blockage enlarges, it may eventually become a visible closed comedone, commonly called a whitehead, or an open comedone, known as a blackhead. If bacteria such as Cutibacterium acnes proliferate within the clogged pore, inflammation can follow, leading to papules, pustules, or deeper nodular acne.
Several contributing factors influence whether microcomedones form and progress. Genetics play a significant role in determining baseline sebum production and inflammatory response. Skincare habits also matter. Overwashing or using harsh cleansers may disrupt the skin barrier, potentially increasing irritation and triggering compensatory oil production. On the other hand, heavy or occlusive skincare products may contribute to clogged pores in individuals prone to comedonal acne. Environmental influences, including humidity and pollution, can also interact with excess oil and debris on the skin’s surface, affecting pore congestion.
Because microcomedones are the earliest stage of acne, prevention strategies often focus on normalizing skin cell turnover and reducing excess sebum before visible lesions appear. Topical retinoids are widely used for this purpose. Retinoids help regulate follicular keratinization and encourage more even shedding of skin cells, which may reduce the formation of clogged pores over time. Over-the-counter retinol products can support mild to moderate comedonal acne, while prescription retinoids are often recommended for more persistent cases. Salicylic acid, a beta hydroxy acid, is oil-soluble and can penetrate into the pore lining, where it may help dissolve accumulated debris and support clearer pores. Benzoyl peroxide is more commonly used for inflammatory acne because it targets acne-associated bacteria, though it may also help prevent progression from microcomedone to inflamed lesion.
Supportive ingredients such as niacinamide may help regulate oil production and calm visible redness, while maintaining the integrity of the skin barrier. Gentle cleansing, consistent sunscreen use, and avoidance of overly occlusive products can further support long-term acne management. Double cleansing techniques may benefit individuals with oily skin who wear makeup or sunscreen daily, but excessive exfoliation should be avoided, as irritation can worsen inflammation and compromise barrier function.
It is important to recognize that acne treatments work gradually because they target the earliest stages of lesion formation. Since microcomedones form weeks before a breakout becomes visible, improvements in blackheads, whiteheads, and inflammatory acne often require consistent use of active ingredients for several weeks or months. Results vary depending on skin type, hormonal influences, and adherence to treatment. Individuals with persistent, scarring, or severe acne may benefit from evaluation by a qualified dermatologist, who can assess underlying contributors and recommend personalized therapies.
Understanding microcomedones highlights why acne management focuses not only on treating visible blemishes but also on preventing the invisible beginnings of clogged pores. By addressing follicular keratinization, excess sebum, and inflammation early, skincare strategies may help reduce the frequency and severity of breakouts over time.