Life is a journey filled with twists and turns, and for many, the path to success is often paved with challenges.
This is particularly true for famous authors who have faced adversity in their lives.
Their stories are not just about the books they wrote but also about the obstacles they overcame to share their voices with the world.
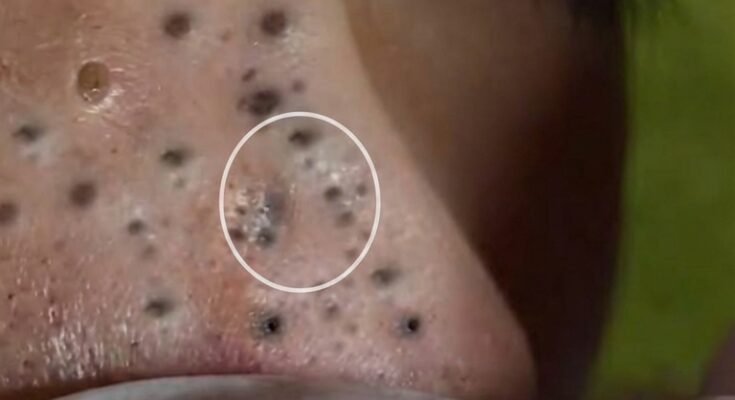
Acne develops through a complex interaction of excess sebum production, abnormal follicular keratinization, clogged pores, microbial activity, and inflammation. Dietary factors have been studied for their potential influence on these biological processes. Certain foods may affect hormonal signaling pathways, particularly insulin and insulin-like growth factor 1, which can stimulate sebaceous gland activity and increase oil production. Elevated insulin signaling may also promote keratinocyte proliferation within the follicle, contributing to microcomedone formation that later develops into blackheads, whiteheads, and inflammatory acne lesions. While diet is not considered the sole cause of acne, emerging research suggests it can act as a modifying factor in individuals who are already prone to breakouts.
High glycemic load diets have received significant attention in acne research. Foods that rapidly raise blood glucose levels may increase insulin and androgen activity, both of which can stimulate sebum production and influence pore clogging. Several clinical studies suggest that lower glycemic diets may help reduce acne severity in some individuals, possibly by improving insulin sensitivity and reducing inflammatory signaling. However, responses vary, and not all patients experience noticeable improvement. Genetics, baseline hormone levels, stress, and existing skincare habits often interact with dietary influences, making acne a multifactorial condition rather than a direct result of specific foods.
Dairy consumption has also been investigated, particularly skim milk. Some observational studies have found associations between higher dairy intake and increased acne prevalence. The proposed mechanism involves bioactive molecules in milk that may affect hormonal pathways linked to sebum production and follicular inflammation. It remains important to interpret these findings cautiously, as association does not prove causation. Many individuals consume dairy without experiencing acne flares, and elimination diets are not universally necessary. When dietary triggers are suspected, gradual and monitored adjustments may be more appropriate than restrictive approaches.
Other dietary components, including highly processed foods and patterns low in antioxidants, have been hypothesized to influence systemic inflammation, which may indirectly affect acne severity. Diets rich in whole grains, vegetables, fruits, and omega-3 fatty acids may support overall skin health by contributing to balanced inflammatory responses and supporting skin barrier function. However, these patterns should be viewed as supportive strategies rather than primary acne treatments.
Because acne fundamentally involves clogged pores, excess oil, and inflammation, evidence-based topical treatments remain central to management. Ingredients such as salicylic acid can penetrate into pores to help dissolve debris and reduce comedones. Retinoids are commonly recommended because they normalize follicular keratinization, reducing the formation of microcomedones that lead to blackheads and whiteheads. Benzoyl peroxide may help decrease acne-causing bacteria and inflammatory lesions, while niacinamide can support the skin barrier and reduce visible redness. In moderate to severe cases, dermatology-guided therapies, including prescription retinoids or hormonal treatments, may be appropriate.
It is also important to recognize that abrupt or extreme dietary restriction can negatively affect overall health and stress levels, which themselves may influence breakouts. Acne improvement related to diet, when it occurs, often develops gradually over several weeks to months. Individuals with persistent, scarring, or hormonally driven acne should consider consulting a qualified healthcare professional to evaluate comprehensive treatment options rather than relying solely on dietary modification.
Current evidence suggests that diet may contribute to acne in certain individuals, particularly through hormonal and inflammatory pathways, but it is rarely the single determining factor. A balanced diet combined with consistent, barrier-supportive skincare and evidence-based acne treatments generally offers a more reliable approach than focusing on any single food group. Educational content within this publication follows evidence-informed dermatologic principles consistent with the standards outlined in the.