Success begins in the mind.
Long before achievements show up in your career, relationships, or finances, they take root in your thoughts.
Training your mind for success is not about pretending challenges do not exist.
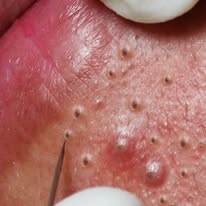
Sunscreen plays a critical role in skin health, yet individuals with acne often worry that it may worsen clogged pores or trigger breakouts. Acne develops through a combination of excess sebum production, abnormal follicular keratinization, bacterial activity, and inflammation. When dead skin cells accumulate inside the follicle and mix with oil, microcomedones form and may progress into blackheads, whiteheads, or inflammatory lesions. Certain sunscreen formulations, particularly those that are thick, highly occlusive, or poorly suited for oily skin, can sit heavily on the surface and potentially contribute to congestion in acne-prone individuals. However, sunscreen itself does not inherently cause acne; formulation choice and skin biology are the determining factors.
Ultraviolet radiation can indirectly worsen acne outcomes. Sun exposure may initially dry out lesions, but it can also increase inflammation, stimulate post-inflammatory hyperpigmentation, and impair the skin barrier. Barrier disruption may lead to increased transepidermal water loss, irritation, and compensatory oil production. In acne-prone skin, maintaining barrier integrity is essential for regulating sebum levels and reducing inflammatory responses. Daily sunscreen use therefore supports overall acne management, especially for individuals using retinoids, benzoyl peroxide, or exfoliating acids that increase photosensitivity.
Non-comedogenic sunscreens are formulated to minimize the risk of clogged pores. While the term “non-comedogenic” is not strictly regulated, it generally indicates that the product has been designed to avoid ingredients commonly associated with pore blockage in susceptible individuals. Lightweight gel, fluid, or lotion textures are often better tolerated by oily skin than thick creams. Formulas labeled oil-free may reduce surface shine, although oil content alone does not determine comedogenicity. Some modern chemical filters are formulated in elegant, fast-absorbing vehicles that leave minimal residue, while mineral sunscreens containing zinc oxide may offer additional anti-inflammatory benefits that can be helpful in acne-prone skin.
Ingredient selection can further improve tolerability. Niacinamide is sometimes included in sunscreen formulations to help regulate sebum production and support barrier function. Silica or other oil-absorbing powders may reduce visible shine throughout the day. Conversely, very heavy emollients or certain waxes, when used in high concentrations, may feel occlusive on oily skin and potentially increase the likelihood of comedonal acne in susceptible individuals. Personal response varies, and a product that works well for one person may not suit another due to differences in genetics, hormone levels, and baseline sebum production.
Cleansing habits also influence whether sunscreen contributes to breakouts. Inadequate removal at the end of the day may allow sunscreen, oxidized sebum, sweat, and environmental pollutants to accumulate within pores. Gentle cleansing, sometimes including a double cleansing method in the evening, may help remove these residues without stripping the barrier. Over-cleansing, however, can irritate the skin and worsen inflammation, so balance remains important.
For individuals actively treating acne, sunscreen compatibility with topical therapies matters. Retinoids help normalize follicular keratinization and reduce microcomedone formation, while salicylic acid penetrates into pores to dissolve debris. Benzoyl peroxide targets acne-associated bacteria. When these treatments are used consistently, they may counterbalance minor congestion risks from cosmetic products. Introducing new sunscreen formulas gradually and patch testing can help identify sensitivity or breakout triggers before widespread application.
Realistic expectations are essential. Even well-formulated non-comedogenic sunscreens may feel different on oily skin compared to dry skin, and some trial and adjustment may be necessary. Avoiding sunscreen due to fear of acne can lead to increased hyperpigmentation, slower healing of acne marks, and long-term photodamage. Selecting lightweight, acne-friendly formulations and maintaining a consistent skincare routine often allows individuals to protect their skin without significantly worsening clogged pores. Persistent or severe acne should be evaluated by a qualified healthcare professional to develop an individualized treatment plan. As emphasized in professional acne education standards, effective acne management requires balancing pore care, inflammation control, and barrier support rather than eliminating protective skincare steps such as sunscreen.