In today’s rapidly changing world, the idea of lifelong learning has taken on new significance.
As we navigate through various stages of our lives, the quest for knowledge and personal growth becomes a continuous journey.
With the advent of artificial intelligence, we are discovering exciting ways to support this journey, making learning more accessible, personalized, and engaging than ever before.
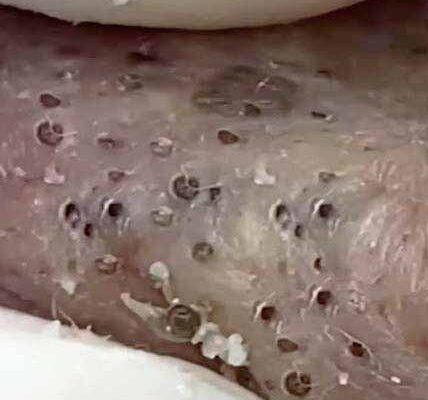
Non-inflammatory acne lesions develop primarily from abnormalities in follicular keratinization and sebum regulation rather than from overt immune-driven inflammation. Within each pore, keratinocytes normally shed in a controlled pattern as sebum travels upward to the skin surface. When this shedding process becomes dysregulated, dead skin cells accumulate and mix with sebum inside the follicle. This mixture can form a microscopic plug known as a microcomedone, which is considered the earliest stage of acne. As the blockage enlarges, it becomes visible as either an open comedone, commonly referred to as a blackhead, or a closed comedone, known as a whitehead. These lesions are categorized as non-inflammatory because they typically lack redness, swelling, and tenderness.
Blackheads form when the follicular opening remains partially open, allowing air exposure. The dark appearance is not due to dirt but rather to oxidation of melanin and lipids within the clogged pore. Whiteheads develop when the follicular opening is closed, trapping the contents beneath the skin surface. Both lesion types reflect impaired cell turnover and excess sebum production, often seen in individuals with oily skin. Although Cutibacterium acnes may be present, the immune response in this stage is limited compared to inflammatory acne, such as papules and pustules.
Hormonal influences frequently contribute to the development of non-inflammatory acne lesions. Androgens stimulate sebaceous glands, increasing oil output and creating an environment where pores are more likely to become congested. Genetic predisposition to larger sebaceous glands or increased keratinocyte cohesion can also increase susceptibility. Skincare habits play a role as well. Heavy, occlusive products, inadequate cleansing, or inconsistent exfoliation may contribute to pore blockage, while excessive or harsh exfoliation can disrupt the skin barrier and paradoxically worsen comedone formation by triggering irritation and rebound sebum production.
Environmental factors, including humidity and pollution, may further influence pore congestion. Sweat combined with sebum and cosmetic residues can accumulate within follicles, particularly when the skin is not cleansed gently and regularly. However, overly aggressive scrubbing does not prevent blackheads and may aggravate barrier dysfunction. The integrity of the skin barrier remains central to maintaining balanced turnover and reducing microcomedone formation.
Evidence-informed treatment for non-inflammatory acne focuses on normalizing follicular keratinization and regulating oil production. Topical retinoids are often recommended because they promote orderly cell turnover within pores and reduce the formation of new comedones over time. Consistent use may gradually decrease both blackheads and whiteheads. Salicylic acid is commonly used as a beta hydroxy acid that penetrates oil and helps loosen compacted debris inside pores. Benzoyl peroxide may be included when mild inflammation is present or to reduce bacterial proliferation, although it is typically more central in inflammatory acne management. Niacinamide may support barrier function and help reduce visible oiliness, improving tolerance to other active skincare ingredients.
Moisturizing is an important component of treatment, even for oily skin. Non-comedogenic moisturizers help maintain barrier stability, which may reduce compensatory sebum production and irritation from active treatments. Sunscreen is also essential, particularly when retinoids or exfoliating acids are used, as these ingredients can increase photosensitivity.
Non-inflammatory acne lesions often respond gradually rather than immediately. Improvement may take several weeks of consistent skincare use. Attempting to extract blackheads manually can damage the follicular wall and increase the risk of inflammation or post-inflammatory hyperpigmentation. For persistent comedonal acne, dermatologists may offer prescription-strength retinoids, chemical peels, or professional extraction performed under sterile conditions.
Understanding non-inflammatory acne lesions highlights the importance of early intervention. Microcomedones can evolve into inflamed papules or pustules if follicular rupture occurs and the immune response intensifies. Addressing clogged pores through balanced, evidence-based skincare may reduce progression and improve overall skin clarity. Individuals with persistent or widespread acne should seek guidance from a qualified healthcare professional to ensure appropriate treatment selection and minimize the risk of long-term skin changes.